How can nasal dysbiosis relate to POTS?
This question sits right at the crossroads of immunology, microbiome science, and autonomic regulation.
A. What is nasal dysbiosis?
Nasal dysbiosis = an imbalance in the microorganisms living in the nasal cavity and sinuses.
A healthy nasal microbiome:
- Is diverse and stable
- Contains protective bacteria (e.g. Corynebacterium, non-pathogenic Staphylococcus)
- Helps regulate local immunity
- Prevents overgrowth of inflammatory or pathogenic microbes
In nasal dysbiosis, you typically see:
- Reduced microbial diversity
- Overgrowth of pro-inflammatory organisms (e.g. Staphylococcus aureus)
- Chronic low-grade inflammation of the nasal mucosa
- Increased immune activation
This can happen after:
- Repeated antibiotics
- Chronic stress
- Viral infections (including COVID)
- Mold exposure
- Immune dysregulation
- MCAS or allergic inflammation
B. How can nasal dysbiosis relate to POTS?
POTS isn’t just a “heart rate problem” — it’s a systemic neuro-immune-vascular condition. Nasal dysbiosis can feed into several of the mechanisms that drive POTS.
Let’s break it down 👇
1. Chronic immune activation → autonomic dysfunction
The nasal cavity is densely connected to the immune system and the nervous system.
Nasal dysbiosis can cause:
- Persistent activation of innate immunity
- Release of cytokines (IL-6, TNF-α, IL-1β)
- Chronic low-grade inflammation
This can:
- Irritate or dysregulate autonomic signaling
- Reduce vagal tone
- Push the system toward sympathetic dominance
→ classic POTS pattern: tachycardia, anxiety-like sensations, poor recovery
2. Mast cell activation (MCAS overlap)
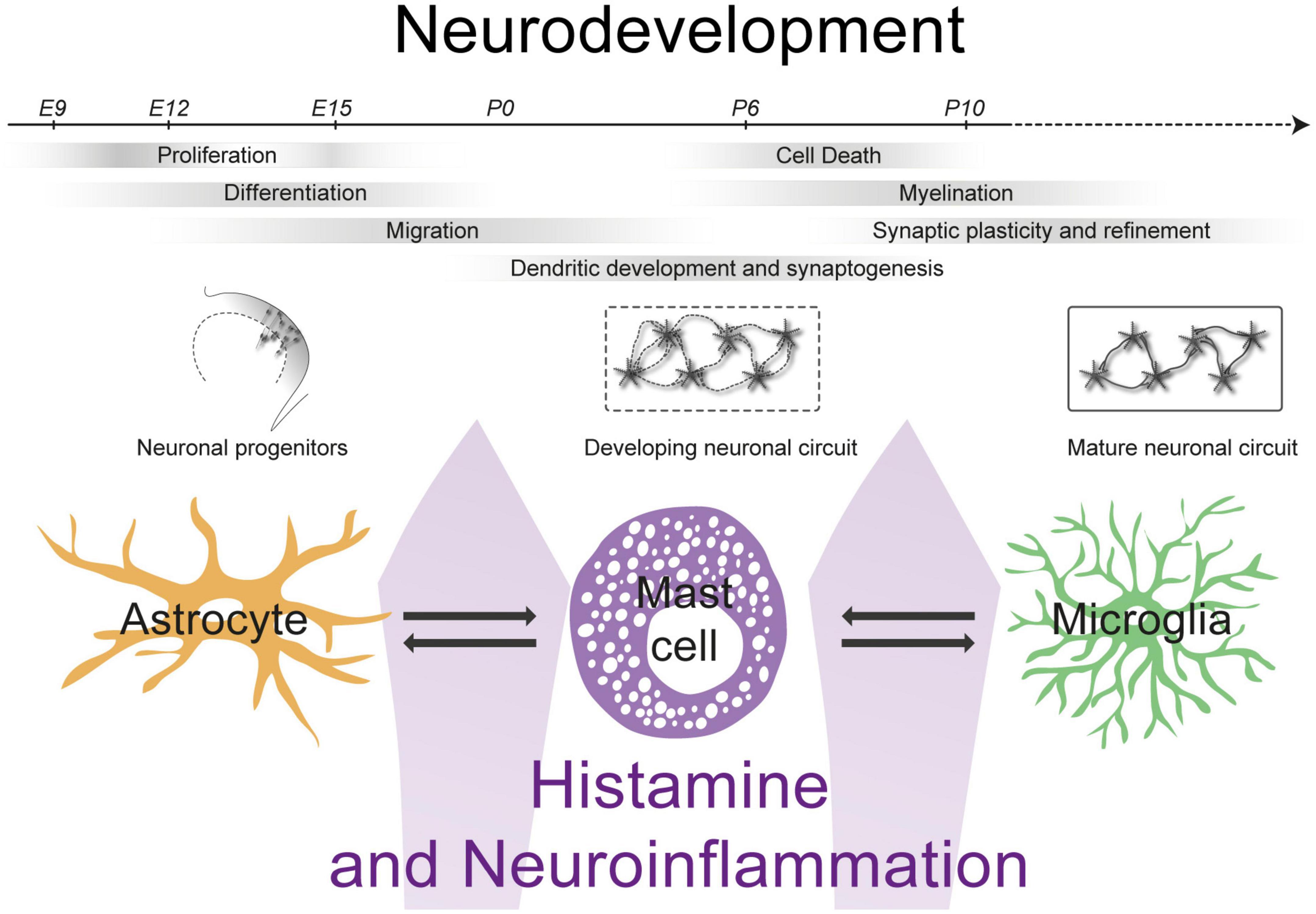
The nasal mucosa is rich in mast cells.
With dysbiosis:
- Mast cells become more reactive
- Histamine and prostaglandins increase
- Local reactions spill into systemic circulation
This can worsen:
- Orthostatic intolerance
- Brain fog
- Flushing
- Palpitations
- GI symptoms
Many people with POTS have MCAS features, and nasal dysbiosis can be one of the triggers keeping mast cells activated.
3. Neuroinflammation via the olfactory–brain route

The nasal cavity is uniquely close to the brain:
- Olfactory nerve
- Trigeminal nerve
- Direct immune-to-brain signaling pathways
Chronic nasal inflammation can:
- Promote neuroinflammation
- Affect hypothalamic and brainstem regulation
- Disrupt autonomic setpoints
This is especially relevant in:
- Post-viral POTS
- Long COVID
- Trauma-sensitized nervous systems
4. Blood vessel dysregulation & nitric oxide imbalance
Certain nasal bacteria influence:
- Nitric oxide (NO) metabolism
- Local vascular tone
Dysbiosis may contribute to:
- Abnormal vasodilation or vasoconstriction
- Poor blood pooling regulation
- Worsened orthostatic symptoms
This connects nasal health to vascular instability, a core feature of POTS.
5. Part of a whole-body dysbiosis pattern

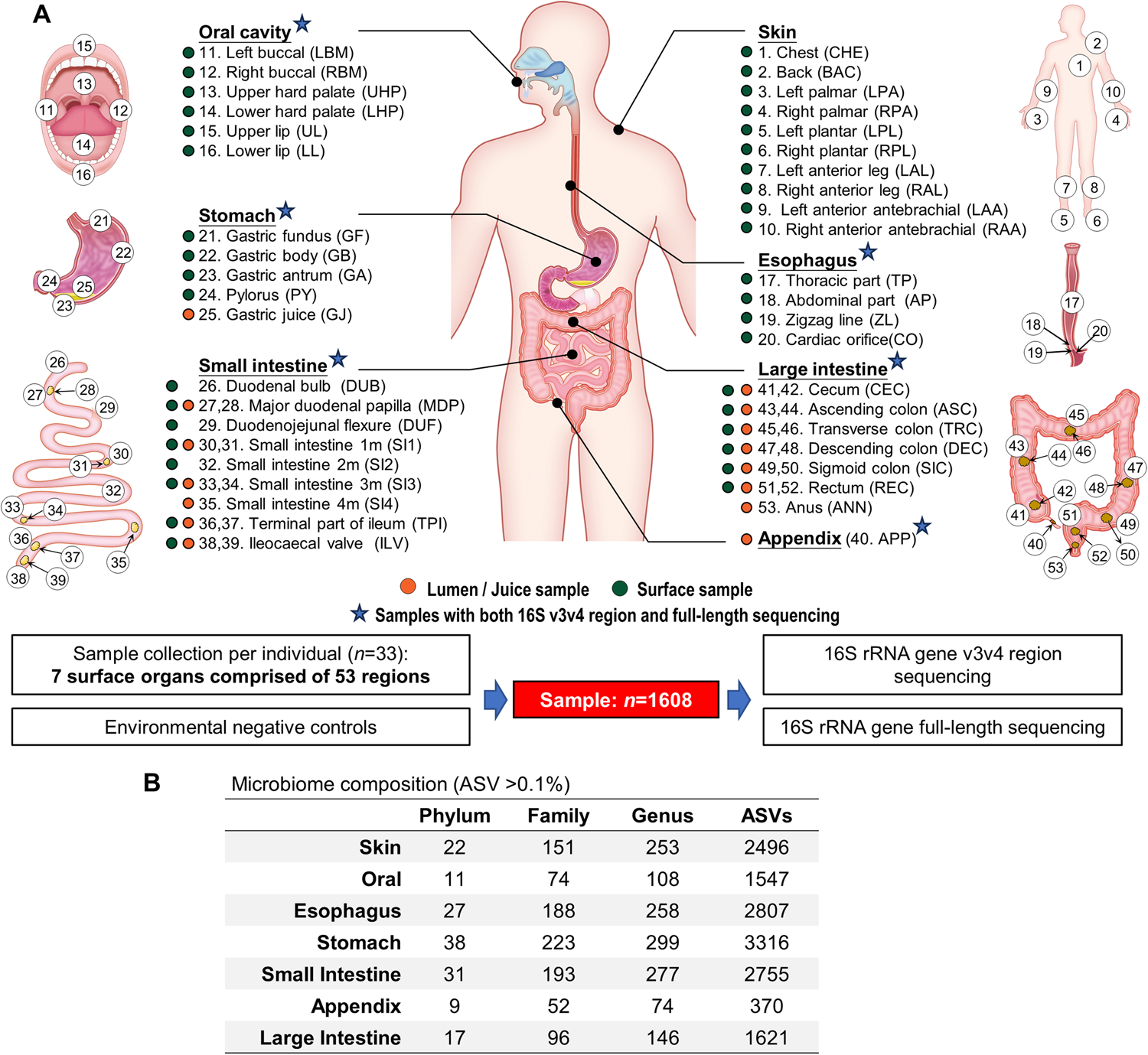
Nasal dysbiosis often coexists with:
- Gut dysbiosis
- Oral microbiome imbalance
- Skin barrier issues
Together, this creates:
- A primed immune system
- Reduced tolerance to stressors
- Increased autonomic reactivity
Think of it as multiple inflamed interfaces constantly poking the nervous system.
Big picture summary
Nasal dysbiosis doesn’t cause POTS on its own, but it can:
- Maintain chronic immune activation
- Exacerbate MCAS
- Increase neuroinflammation
- Reduce vagal tone
- Worsen orthostatic intolerance
In people with:
- Neurodivergence
- Trauma history
- Post-viral illness
- Hypermobility / connective tissue fragility
…it can be a meaningful amplifier.



